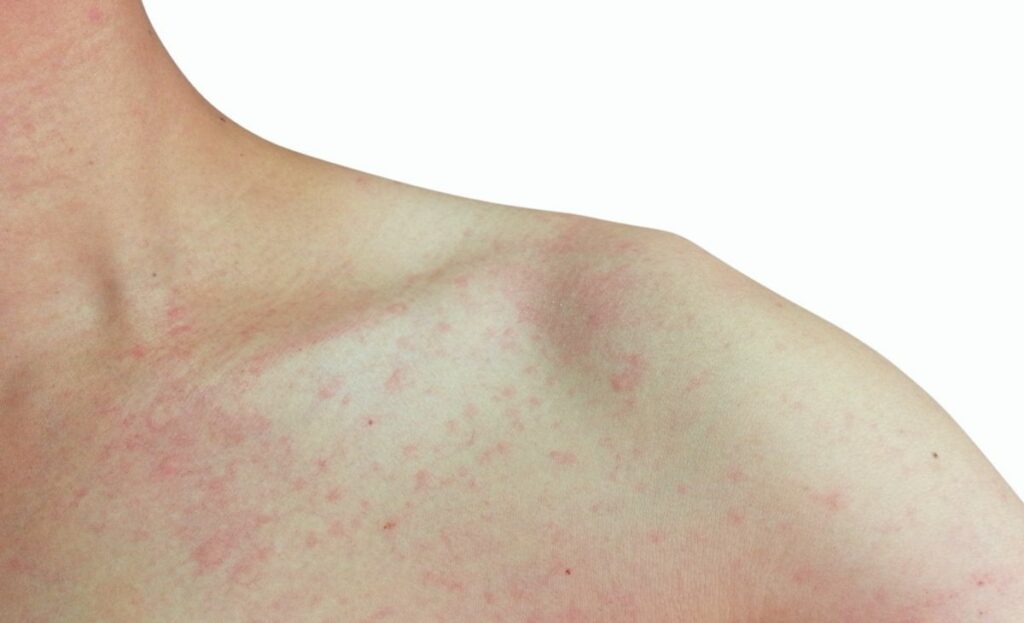
The skin is susceptible to many skin conditions, including inflammatory ones. These can limit people’s lives over a short period, or for years. Dr Ravi Ratnavel is a leading UK dermatologist and in this article, he shares his professional expertise so that you can understand inflammatory skin conditions, their causes, treatment and more. Inflammatory skin disease is commonly known as a “skin rash”.
What is an inflammatory skin disease (skin rash)?
“Inflammatory skin disease” is a term that covers a very large number of skin conditions. These conditions can arise from many different causes and they present as skin eruptions and rashes, which can be self-limiting over a few weeks or take a chronic course lasting many years. Their common characteristic is a change in colour (and sometimes texture) of the skin.
At the tissue level, there are varying degrees of accumulation of normal white blood cells which are responsible for immunity against infections. This process can result in alteration of the appearance of the skin e.g. it can produce papules (tiny bumps), pustules (pus spots) and flat patches of pigment change (macules). Also, there may be dilatation of microscopic blood vessels in the skin which will manifest as redness (erythema).
What are the most common inflammatory skin conditions?
The most common inflammatory skin conditions include chronic disorders such as eczema, psoriasis, acne, folliculitis and allergic urticaria.
They also cover skin rashes which may be infective in origin e.g. those associated with the coronavirus COVID-19 and common childhood viruses such as molluscum contagiosum and chickenpox.
What are the less common inflammatory skin conditions?
More rarely, there are food-induced allergic skin reactions such as dermatitis herpetiformis, which is related to gluten allergy. Another important group are drug eruptions, which are caused not only by prescribed and over the counter medications, but also by herbal preparations and dietary supplements.
Can inflammatory skin diseases can be prevented?
Regular use of emollients (moisturising treatments) is important in reducing flare-ups of eczema. In acne sufferers, avoiding comedogenic (oil-based) products such as hair wax and some types of make-up is important.
Most skin conditions are events without preventable causes and are related to individual genetic and immunological make-up. Good personal hygiene reduces the risk of superficial skin infections.
In patients with skin conditions such as eczema and urticarial, avoiding relevant food and contact allergens can help in a minority.
Can inflammatory skin conditions resolve on their own?
Many acute conditions such as lichen planus and pityriasis rosea (which result from autoimmunity and possibly infection) are self-resolving. Most teenage acne and childhood eczema also resolve spontaneously with time.
Are inflammatory skin diseases curable?
Chronic disorders such as psoriasis and urticaria can go through good phases and bad ones. However, they cannot be cured in the way an infection can. The expectation should be control rather than cure. However, targeted medical treatment can certainly offer relief of associated symptoms such as itchiness and pain, as well as offer visual improvement. It is also helpful to identify and address any triggers to the flare-ups which occur.
What are the best treatment options for inflammatory skin diseases?
Effective treatment is directed by the cause. Accurate medical diagnosis forms the cornerstone of proper treatment and this can prove challenging to primary care practitioners, owing to the many hundreds of skin conditions which can look like each other to the non-specialist.
Many common skin conditions respond to anti-inflammatory topical steroid creams, but it’s important to both select the right strength of the prescribed product and to exclude infection before these are used.
To learn how you can benefit from Dr Ratnavel’s highly professional and personalised patient care, simply message or phone his practise today.
